Can Stimulating One Nerve Really Fix Your Gut?
That bloated, sluggish feeling after meals. The knot in your stomach when stress hits. The way your gut seems to have a mind of its own. What if these digestive struggles all traced back to one nerve — your vagus nerve — and what if stimulating it could help? Current research on vagus nerve stimulation for digestive wellness is extremely limited, but the theoretical connection between this nerve and gut function is fascinating scientists.
How Does the Vagus Nerve Connect to Your Gut?
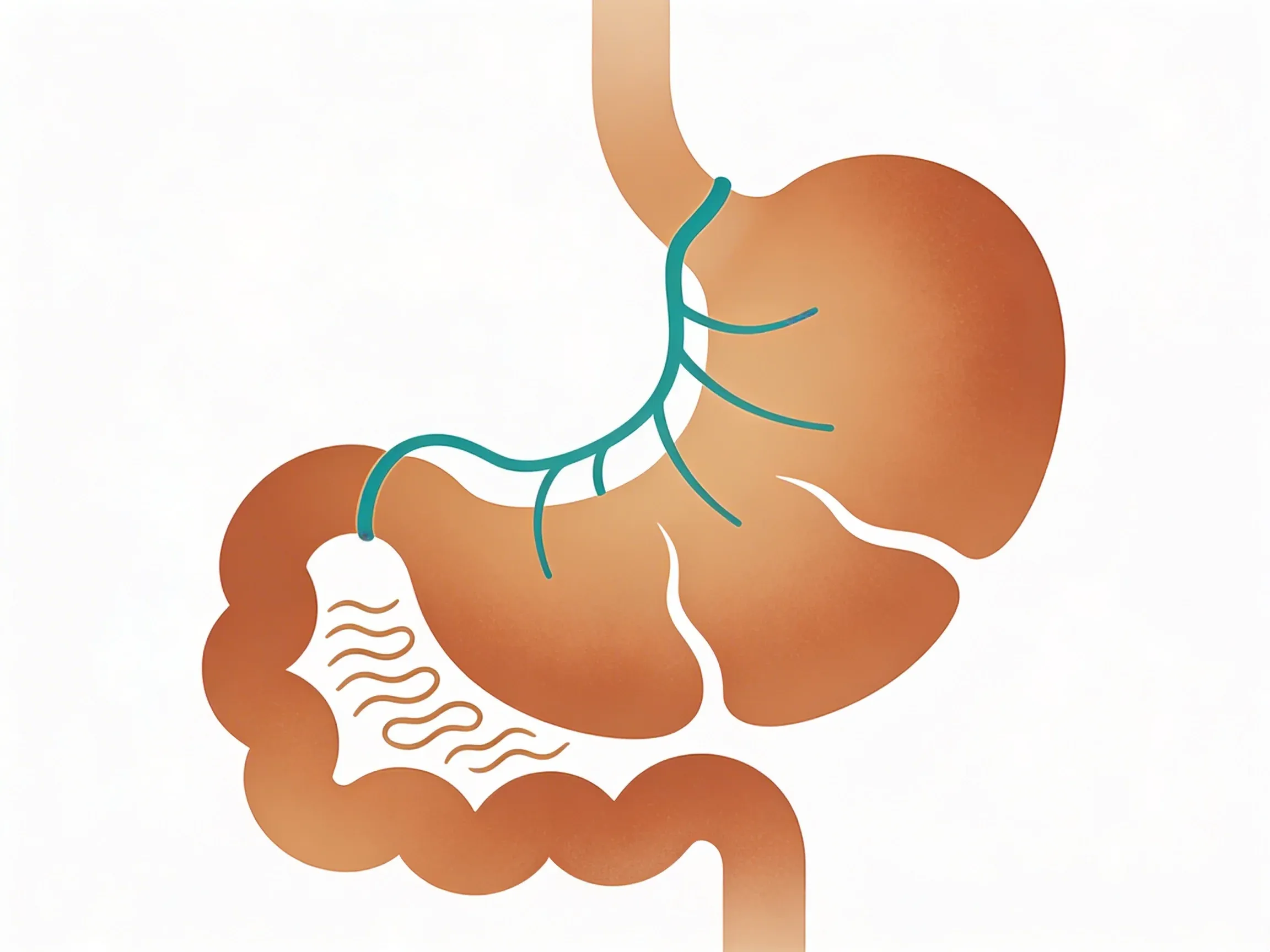
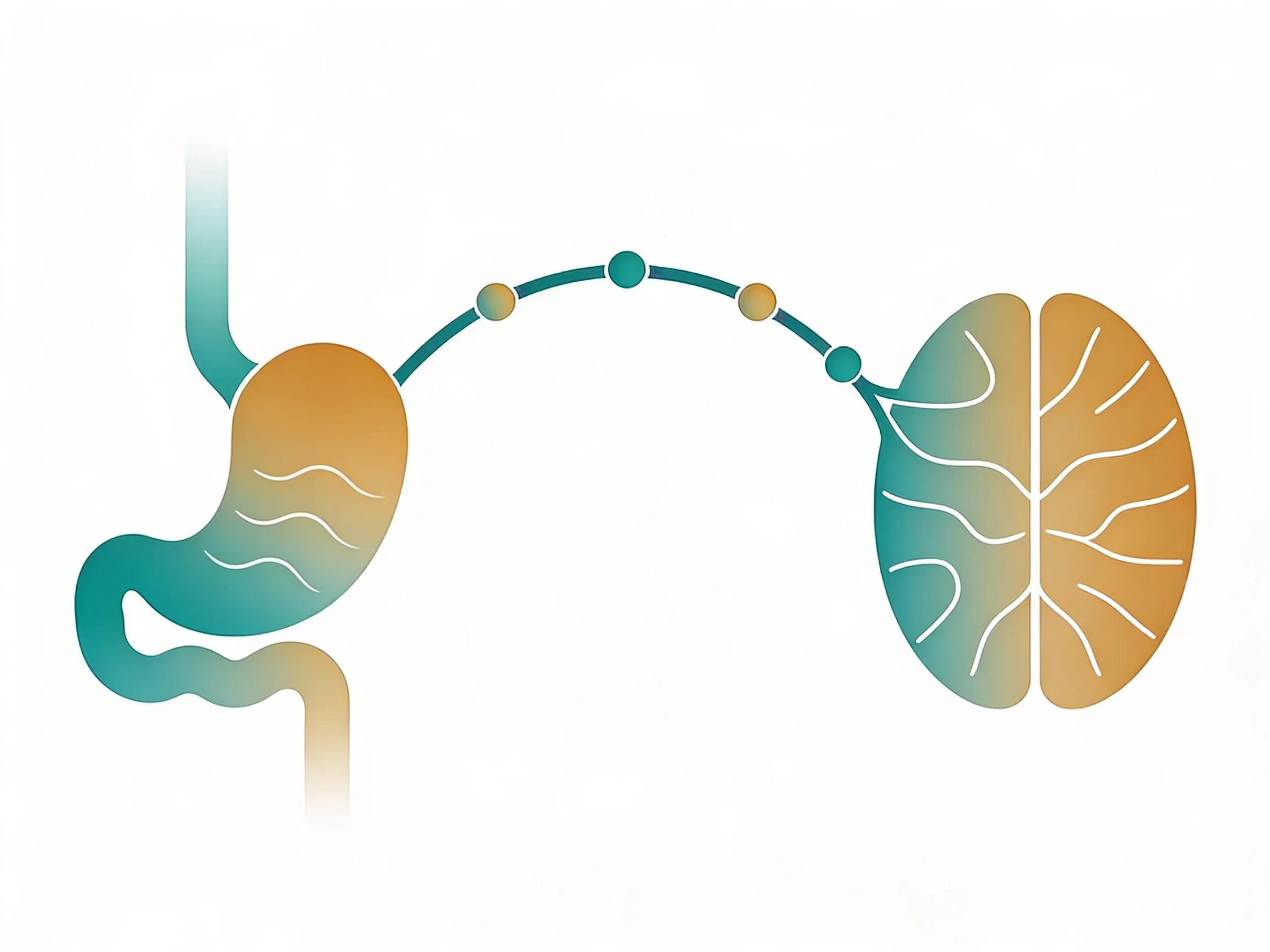
Your vagus nerve is the main highway between your brain and digestive system. This long nerve runs from your brainstem all the way down to your abdomen. It touches your stomach, liver, and intestines along the way.
Think of it like a control center for digestion, like a conductor telling the orchestra when stomach acids should flow and intestinal muscles should contract. The vagus nerve tells your stomach when to make acid. It controls how fast food moves through your gut. And it helps manage inflammation in your digestive tract.
This connection works both ways. Your gut sends signals up to your brain through the vagus nerve too. That's why you might feel nauseous when stressed or get "butterflies" when nervous.
Key takeaway: Your vagus nerve doesn't just carry messages from brain to gut — it actively shapes whether your body prioritizes digestion or stress response.
When your vagus nerve is working well, it activates your parasympathetic nervous system. This is your "rest and digest" mode. Your body shifts resources toward digestion and repair.
What Does Current Research Say About VNS for Digestion?
Here's the thing: there's very little research on vagus nerve stimulation specifically for digestive wellness.
Most vagus nerve stimulation studies focus on conditions like epilepsy and depression. These use implanted devices that deliver electrical pulses directly to the nerve. The FDA has approved these for certain medical conditions.
But research on non-invasive vagus nerve stimulation for gut health? That's where things get thin. We don't have large-scale studies looking at whether stimulating the vagus nerve through the skin helps with everyday digestive concerns like bloating or discomfort.
The research that does exist is mostly theoretical. Scientists understand how the vagus nerve affects digestion. They know that activating the parasympathetic nervous system should help with digestive function. But proving that vagus nerve stimulation devices actually improve gut comfort? We're not there yet.
Given these research gaps, let's explore why scientists think VNS might help digestion.
Why Might VNS Theoretically Help Your Gut?
Even without solid clinical evidence, there are logical reasons why vagus nerve stimulation might support digestive wellness.
First, stimulating the vagus nerve should activate your parasympathetic nervous system. This is the state where your body prioritizes digestion over stress responses. Your stomach produces more acid. Your intestines move food along more smoothly.
Second, the vagus nerve helps control inflammation throughout your digestive tract. When this nerve fires properly, it may help keep gut inflammation in check. This could theoretically support overall digestive comfort.
Here's where it gets interesting: stress wreaks havoc on digestion. Many people notice their gut issues get worse during stressful periods. If vagus nerve stimulation helps manage stress responses, it might indirectly support digestive function too.
But remember: these are theoretical benefits. We need actual studies to know if vagus nerve stimulation devices deliver these effects in real people.
What About Natural Vagus Nerve Activation?
While we wait for more research on devices, there are natural approaches worth exploring.
You don't need a device to potentially influence your vagus nerve. Several natural techniques may help activate this nerve:
Try this 2-minute gut-calming technique:
1. Sit comfortably and place one hand on your chest, one on your belly
2. Inhale slowly through your nose for 4 counts (belly should rise more than chest)
3. Exhale slowly through your mouth for 6-8 counts
4. Repeat for 10 breaths
5. Notice if your stomach feels more relaxed
Other natural approaches include:
- Cold exposure: Cold water on your face or neck for 30-60 seconds may activate the dive reflex
- Gargling: The vibrations can stimulate vagal pathways
- Humming or singing: Similar vibration effects
- Gentle neck stretches: May help with vagal tone
Again, research on these techniques for digestive health specifically is limited. But they're low-risk approaches that many people find relaxing. And relaxation generally supports better digestion.
Some people also use non-invasive vagus nerve stimulation devices. These typically clip to your ear and deliver mild electrical pulses. The theory is that they can provide more consistent stimulation than breathing exercises alone.
Are There Risks to Consider?
The reality check? Vagus nerve stimulation techniques are generally considered safe for most healthy people. But there are some important considerations.
If you have any chronic digestive condition, talk to your doctor before trying vagus nerve stimulation. This includes conditions like IBS, Crohn's disease, or chronic gastritis. These need proper medical management.
For electronic stimulation devices, make sure they're from reputable manufacturers. Avoid using any device near your neck if you have heart rhythm problems or a pacemaker.
Natural techniques like deep breathing and cold exposure are very low risk. But if you have any serious health conditions, check with your healthcare provider first.
But there's a catch: the biggest risk might be relying on vagus nerve stimulation instead of addressing underlying digestive issues. If you have persistent gut problems, see a gastroenterologist. Don't use VNS as a substitute for proper medical evaluation.