6 Simple Vagus Nerve Exercises to Support Digestive Comfort
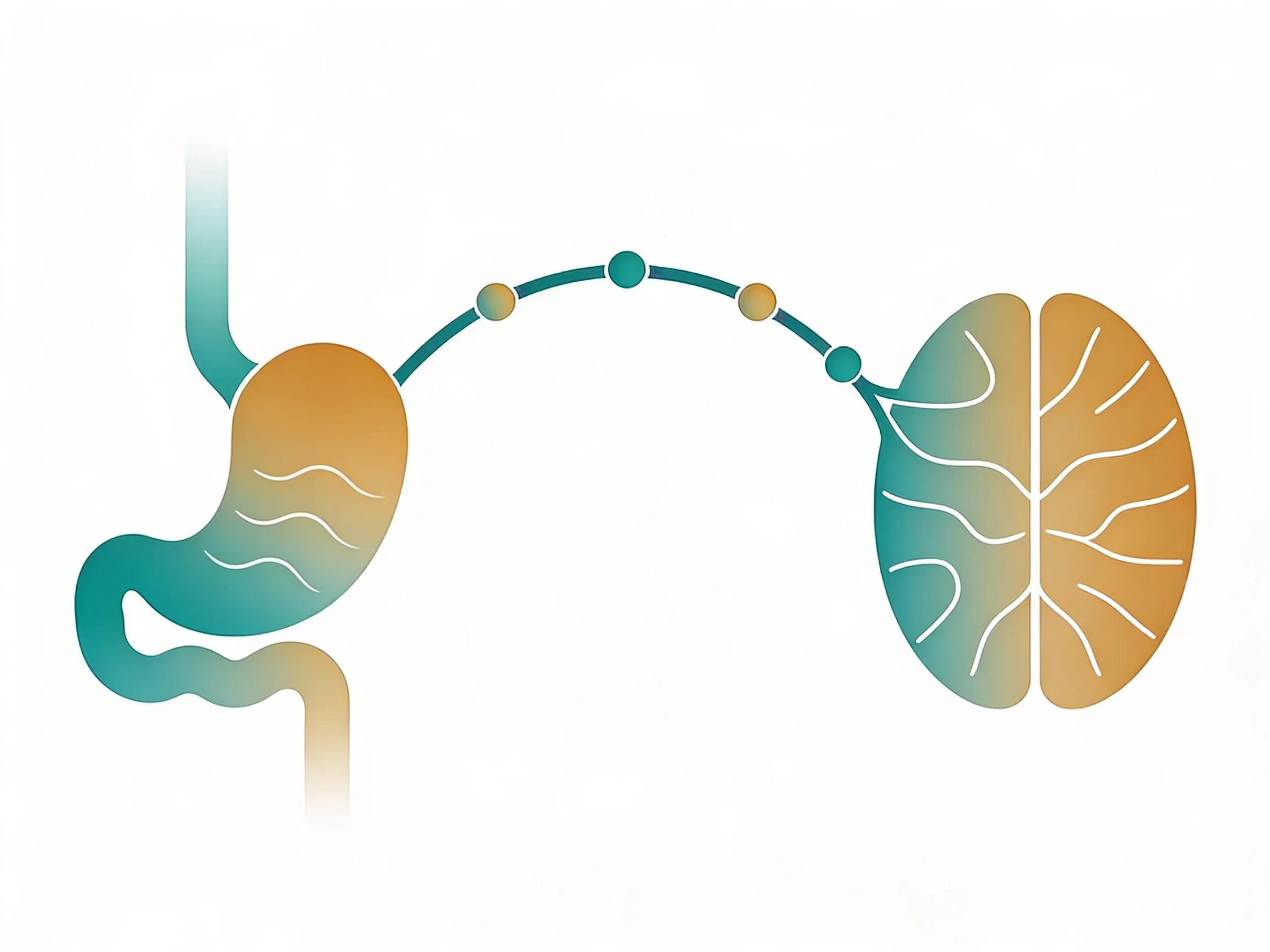
That uncomfortable bloated feeling after meals? The sensation that food is just sitting in your stomach like a heavy stone? These digestive struggles might stem from poor communication between your brain and gut. Your vagus nerve acts as the main communication highway between these two areas, helping regulate digestion, nutrient absorption, and the smooth movement of food through your digestive tract. Research suggests these techniques may help activate this nerve to support overall digestive comfort and function1.
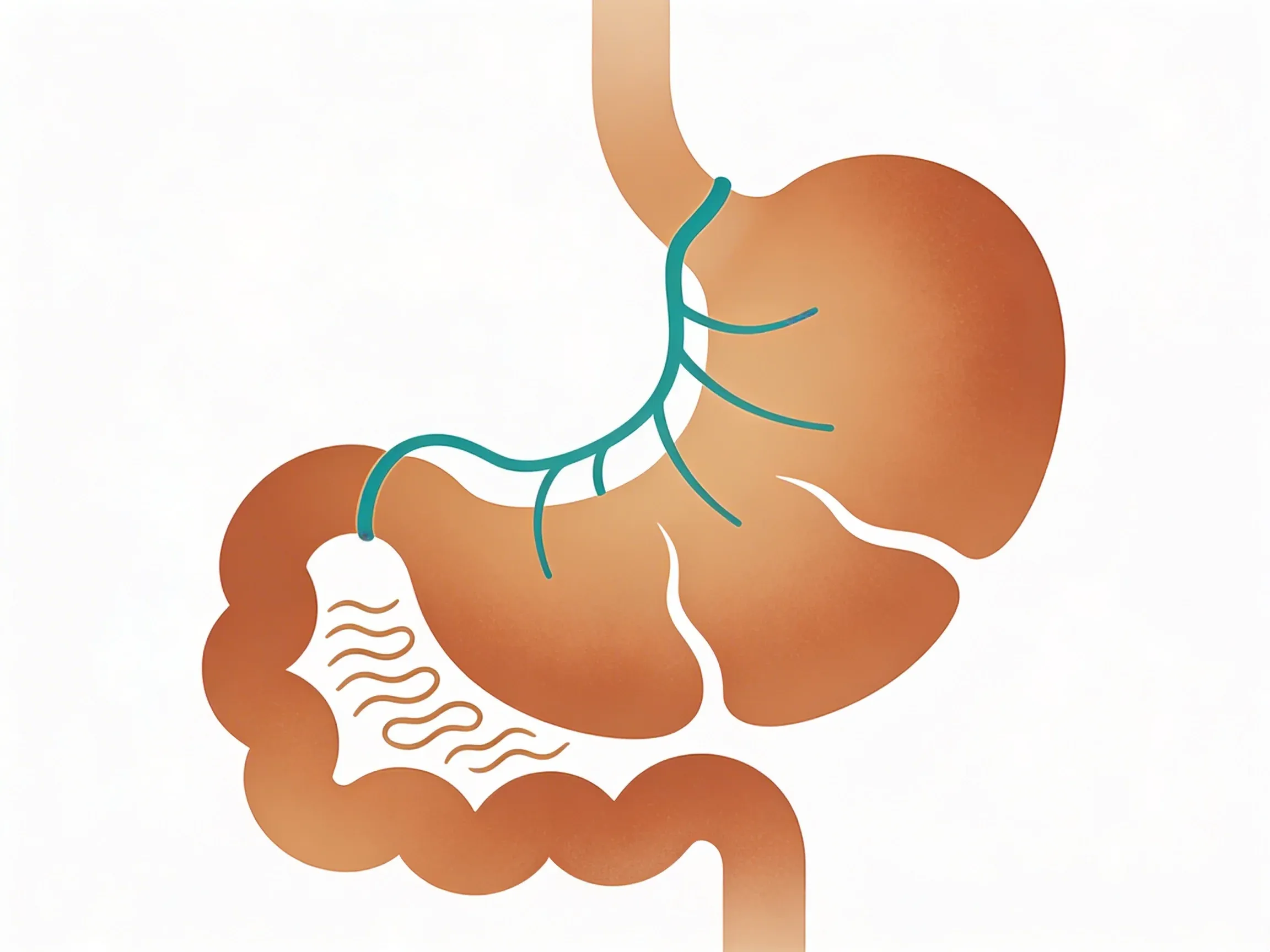
How Does the Vagus Nerve Affect Your Digestive System?
Think of your vagus nerve as a telephone line between your brain and belly. When this connection is strong and clear, your brain can send crisp signals to your digestive organs -- like a high-quality phone call with perfect sound. Your stomach gets clear instructions to produce the right amount of acid. Your intestines receive proper signals to move food along at a healthy pace. And your gut can effectively absorb vitamins and minerals from meals.
But when vagal tone is poor, it's like having a phone line full of static. The signals become weak and garbled. Your stomach might not get the message to start producing digestive juices. Your intestines might slow down or speed up at the wrong times. This communication breakdown can leave you with bloating, gas, or that uncomfortable "food just sitting there" feeling after eating.
This long nerve starts in your brainstem and travels down to your abdomen, making it the main controller of your "rest and digest" mode.
1. Deep Breathing: The Foundation Practice
Research suggests deep breathing may work, and here's the proposed mechanism. Deep breathing exercises may help stimulate your vagus nerve by activating your parasympathetic nervous system -- the branch that handles "rest and digest" functions.
When you take slow, deep breaths, your diaphragm moves up and down. This movement creates gentle pressure that may help stimulate the vagus nerve. The nerve then sends calming signals to your digestive organs, potentially helping them work more smoothly.
Try this before meals:
Pre-meal breathing reset:
1. Sit comfortably and place one hand on your chest, one on your belly
2. Breathe in slowly through your nose for 4 counts, letting your belly rise
3. Hold for 2 counts
4. Exhale slowly through your mouth for 6 counts
5. Repeat 5 times
Many people find this simple practice helps them feel more relaxed before eating. And when your nervous system is calm, digestion tends to work better.
2. Gargling: Building on Breath Work
Once you've established a breathing practice, gargling adds another layer of vagal stimulation. This might sound odd, but gargling provides consistent vibration that may activate your vagus nerve. Think of it like tuning a guitar string -- the vibrations from gargling can help calibrate your vagus nerve to function more effectively. The nerve runs near your throat, and these vibrations may stimulate it directly, helping prepare your entire digestive system for optimal function.
To try it:
- Use plain water or a mild saltwater solution
- Gargle for 30 seconds, making sure you feel the vibration in your throat
- Do this 2-3 times, about 10 minutes before eating
- Some people prefer to hum loudly instead, which creates similar vibrations
The key is creating that vibratory sensation that reaches the vagus nerve pathways near your throat.
3. Gentle Massage: Physical Support for Nerve Function
After activating your vagus nerve through breathing and throat vibrations, gentle massage can provide additional physical support. Gentle massage applied to areas where the vagus nerve passes -- like your neck, throat, and abdomen -- may provide helpful stimulation. You're not trying to massage the nerve directly (that's not possible). Instead, you're encouraging blood flow and relaxation in areas where the nerve travels.
Here's the thing: massage may work on more than just your muscles. It appears to signal your autonomic nervous system to shift into a calmer state.
Try these simple massage techniques:
Neck massage: Use gentle circular motions along the sides of your neck, moving from behind your ears down toward your collarbone.
Abdominal massage: Place your hands on your belly and make slow, clockwise circles. This follows the natural direction of digestion.
Throat massage: Gently stroke from your chin down to your collarbone, using light pressure.
Spend 2-3 minutes on each area. The goal is relaxation, not deep pressure.
4. Gentle Movement: Combining Breath and Motion
Building on the foundation of breathing and physical stimulation, gentle movement may enhance vagal nerve activity and support overall digestive comfort. Research on contemplative practices suggests that slow, rhythmic movement combined with controlled breathing may activate the parasympathetic nervous system through respiratory vagal pathways2. These practices combine movement with mindful breathing, which creates a double benefit for your vagus nerve.
The key word here is "gentle." Intense exercise actually activates your sympathetic nervous system -- the "fight or flight" mode that can slow digestion. But gentle, flowing movements do the opposite.
Yoga poses that involve twisting or gentle compression of the abdomen seem particularly helpful. Think of poses like:
- Seated spinal twist
- Knees to chest
- Child's pose
- Cat-cow stretches
Tai chi offers similar benefits through its slow, coordinated movements combined with deep breathing. The rhythmic nature of these practices may help regulate the nerve signals that control gut function.
5. Sound Vibrations: Vocal Techniques for Deeper Activation
To further enhance the vibrational effects you've created through gargling, vocal techniques can provide even deeper stimulation. Chanting sounds like "om" may provide vagal stimulation through vocal vibrations, especially when combined with other relaxation practices. The vibrations you create when chanting travel through your throat and chest, potentially stimulating vagus nerve pathways.
This isn't just about the sound itself. It's about the combination of controlled breathing, vibration, and the meditative focus that chanting requires.
To try vocal vibration:
- Take a deep breath and chant "om" or "ahh" for as long as your exhale lasts
- Focus on feeling the vibration in your throat and chest
- Repeat 5-10 times
- Some people prefer humming, which creates similar vibrations with less effort
The vibration is what matters most. Pick whatever sound feels comfortable and natural for you.
6. Vagus Nerve Stimulation Devices: Technology as Support
While the manual techniques above offer wonderful benefits, they do require daily practice, mindful attention, and consistent effort. Some people struggle to maintain regular routines or prefer more predictable stimulation throughout their day. Others find it challenging to remember breathing exercises or set aside time for massage techniques.
For these reasons, some people explore technological alternatives. A 2025 systematic review of VNS for gastrointestinal disorders found that non-invasive devices -- including transcutaneous auricular vagal nerve stimulation (tVNS) -- showed promising early results across conditions like IBS and functional dyspepsia3. However, the authors noted that most studies were small, and more research is needed to establish optimal protocols and long-term effects.
These devices work differently than the natural techniques we've covered -- they provide more targeted, consistent stimulation without requiring you to remember daily breathing exercises or massage routines.
Some people find devices helpful as a foundation while they build habits around manual techniques. Others prefer the mindful, intentional aspect of practices like breathing and gargling. The choice often comes down to lifestyle -- devices work passively while you go about your day, while manual techniques require dedicated time but offer the added benefit of stress reduction.
If you're considering a device, look for ones specifically designed for wellness use. And remember: these are supportive tools, not medical treatments.
How Can You Tell if These Techniques Are Working?
Your body will give you feedback, but it might take a few weeks of consistent practice to notice changes. Here's what to watch for and why each sign matters:
- Feeling more relaxed during meals -- When your vagus nerve activates the parasympathetic "rest and digest" state, your body redirects blood flow toward your digestive organs. That calm sensation during eating is your nervous system shifting gears.
- Less bloating or gas after eating -- Bloating often results from sluggish stomach emptying. Stronger vagal signals may help your stomach produce digestive acids on schedule and move food into the small intestine at a healthy pace.
- Better appetite regulation -- Your vagus nerve carries fullness signals from your gut to your brain. When this pathway works well, you feel hungry at regular times and recognize satiety earlier, rather than swinging between no appetite and sudden hunger.
- Improved bowel movement regularity -- Your vagus nerve triggers the wave-like muscle contractions (peristalsis) that move food through your intestines. More consistent vagal tone may mean more predictable digestive timing.
- Less of that "food sitting in my stomach" sensation -- This heavy feeling often points to slow gastric motility. When vagal signals reach your stomach clearly, it contracts more effectively to break down and pass food along.
Keep in mind that digestive improvements often happen gradually. Your vagus nerve tone builds over time with regular practice, similar to building muscle strength. Most people notice subtle shifts in the first 2-3 weeks, with clearer changes developing over 1-2 months.
For the best results, try combining 2-3 of these techniques rather than relying on just one. Many people find success with a pre-meal breathing routine plus one other method like gentle massage or gargling.